Physical exercise in older patients with heart failure
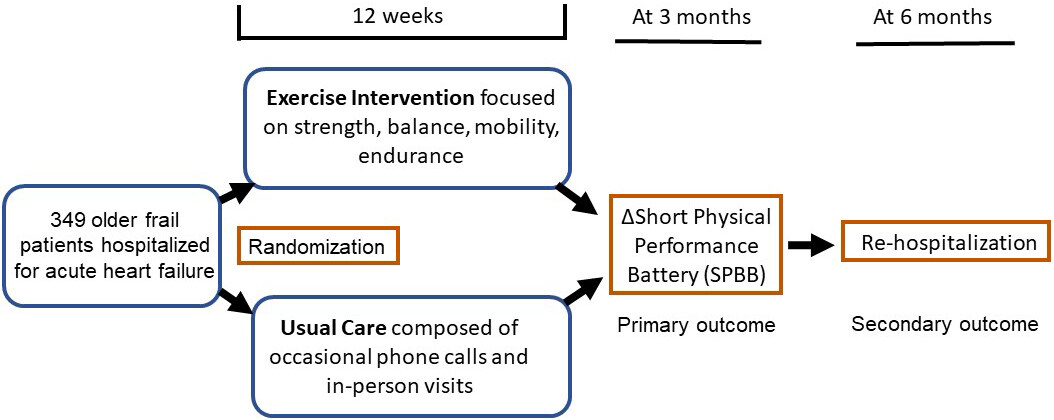
Patients admitted for acute decompensated heart failure (ADHF) demonstrate substantially high in-hospital morbidity and mortality and exhibit worsening fatigue, significant activity limitations, and exercise intolerance[1]. In this patient population, exercise tolerance and, more specifically, exercise capacity may be a better prognostic indicator than cardiac function[2]. Despite this, most of the available clinical guidelines do not emphasize physical dysfunction and frailty that are highly prevalent in patients with ADHF. The rehabilitation therapy in older acute heart failure patients (REHAB-HF) was designed to fill this gap[3]. The goal of the clinical trial was to evaluate the efficacy of an individualized exercise rehabilitation program compared with a usual care group in 349 patients hospitalized with heart failure regardless of ejection fraction (see Figure 1). Exercise utilized was not a standard cardiac rehabilitation program. The intervention started as soon as patients were hospitalized and gradually transitioned into the outpatient setting three days a week. This is a ground-breaking approach as performing exercise training during ADHF was generally considered highly risky due to severely impaired exercise tolerance. The exercise prescription was custom-tailored to individual patients based on functional performance level and emphasized improvements in four key components of physical fitness: endurance, mobility, strength, and balance. Home-based exercises composed of low-intensity walking were also prescribed on non-program days. Considering that the participants had multiple comorbid conditions limiting mobility and reducing exercise compliance, exercise adherence was excellent at 82% for three months. A gradual transition to self-directed home-based programs may have removed some of the crucial barriers such as lack of transportation, financial problems, and the need to care for dependent spouse and acted to enhance exercise adherence. The high exercise adherence was particularly impressive given that participation in exercise-based cardiac rehabilitation remains very low in clinical practice worldwide, with substantially high dropout rates even after enrollment despite concrete evidence demonstrating the clinical and functional benefits[4].
Figure 1. The overall clinical trial design of the rehabilitation therapy in older acute heart failure patients (REHAB-HF) study.
Significant improvements were noted in all physical function domains using the primary outcome measure of the short physical performance battery score. Functional improvements were also seen in the 6-min walk distance and gait speed. The magnitude of the increase in the 6-min walk distance was ~100m, which is translated to a large improvement in the clinical status of patients with heart failure[5]. These results are certainly encouraging in creating a better quality of life for a number of older adults who suffer from acute heart failure. However, mortality was much greater in the exercise group than in the control group, and there was no group difference in all-cause and heart failure-related hospital re-admission. These findings may be disappointing given the significant improvements observed in multiple elements of physical function. However, this is not surprising as the effects of exercise-based cardiac rehabilitation on complex clinical outcomes remain highly controversial in patients with heart failure[6]. It is unclear what explains the discrepant results, but it may be related to acute (adverse) responses to exercise bouts as some patients with ADHF respond to exercise with heightened oxidative stress and exhibit a poor prognosis[7].
“Exercise is medicine” is a global health initiative to promote physical activity in clinical care. The results of the REHAB-HF study provide further confirmation of this initiative. It should be noted that exercise is different from drugs. There is no standard dose that fits with every patient. Unlike drug therapy, there are no non-responders when the exercise dose is set correctly to improve cardiovascular fitness, at least in healthy adults[8]. Exercise is similar to drugs as it has a variety of choices to enhance conditions and performance. In recent years, exercise modalities constructed for athletes are being adapted for various patient populations, including heart failure. For instance, high-intensity interval training has emerged as an effective and safe exercise modality for patients with heart failure and heart transplants[9]. Blood flow restriction training (exercise training technique that combines low-intensity resistance exercise with blood flow occlusion to the arms and legs) is prescribed to older frail patients awaiting abdominal cancer surgery[10] and may be applied to patients with heart failure soon. The overall exercise program constructed by the REHAB-HF study is consistent with this concept. It is innovative and encompasses the interplaying fields of cardiology, geriatrics, and kinesiology. The exercise program was feasible in the research setting and highly effective in enhancing physical function even for frail elderly patients with acute heart failure. However, as the overall intervention program was very resource- and personnel-intensive, the applicability of the REHAB-HF exercise protocol to routine cardiac rehabilitation settings remains unclear. For the same reason, long-term adherence to the program needs to be investigated further.
DECLARATIONS
Authors’ contributionsThe author contributed solely to the article.
Availability of data and materialsNot applicable.
Financial support and sponsorshipNone.
Conflicts of interestThe author declared that there are no conflicts of interest.
Ethical approval and consent to participateNot applicable.
Consent for publicationNot applicable.
Copyright© The Author(s) 2022.
REFERENCES
1. Kurmani S, Squire I. Acute heart failure: definition, classification and epidemiology. Curr Heart Fail Rep 2017;14:385-92.
2. Mancini DM, Eisen H, Kussmaul W, Mull R, Edmunds LH Jr, Wilson JR. Value of peak exercise oxygen consumption for optimal timing of cardiac transplantation in ambulatory patients with heart failure. Circulation 1991;83:778-86.
3. Kitzman DW, Whellan DJ, Duncan P, et al. Physical rehabilitation for older patients hospitalized for heart failure. N Engl J Med 2021;385:203-16.
4. Thomas RJ, Beatty AL, Beckie TM, et al. Home-based cardiac rehabilitation: a scientific statement from the american association of cardiovascular and pulmonary rehabilitation, the American Heart Association, and the American College of Cardiology. Circulation 2019;140:e69-89.
5. Spertus J, Peterson E, Conard MW, et al. Cardiovascular Outcomes Research Consortium. Monitoring clinical changes in patients with heart failure: a comparison of methods. Am Heart J 2005;150:707-15.
6. Taylor RS, Walker S, Smart NA, et al. ExTraMATCH II Collaboration. Impact of exercise-based cardiac rehabilitation in patients with heart failure (ExTraMATCH II) on mortality and hospitalisation: an individual patient data meta-analysis of randomised trials. Eur J Heart Fail 2018;20:1735-43.
7. Shibata A, Izumiya Y, Yamaguchi Y, et al. Increased oxidative stress during exercise predicts poor prognosis in patients with acute decompensated heart failure. ESC Heart Fail 2021; doi: 10.1002/ehf2.13538.
8. Montero D, Lundby C. Refuting the myth of non-response to exercise training: 'non-responders' do respond to higher dose of training. J Physiol 2017;595:3377-87.
9. Masarone D, Melillo E, Petraio A, et al. Exercise-based rehabilitation strategies in heart transplant recipients: focus on high-intensity interval training. Clin Transplant 2021;35:e14143.
Cite This Article
Export citation file: BibTeX | RIS
OAE Style
Tanaka H. Physical exercise in older patients with heart failure. J Cardiovasc Aging 2022;2:2. http://dx.doi.org/10.20517/jca.2021.23
AMA Style
Tanaka H. Physical exercise in older patients with heart failure. The Journal of Cardiovascular Aging. 2022; 2(1): 2. http://dx.doi.org/10.20517/jca.2021.23
Chicago/Turabian Style
Tanaka, Hirofumi. 2022. "Physical exercise in older patients with heart failure" The Journal of Cardiovascular Aging. 2, no.1: 2. http://dx.doi.org/10.20517/jca.2021.23
ACS Style
Tanaka, H. Physical exercise in older patients with heart failure. J. Cardiovasc. Aging. 2022, 2, 2. http://dx.doi.org/10.20517/jca.2021.23
About This Article
Copyright
Data & Comments
Data

 Cite This Article 9 clicks
Cite This Article 9 clicks












Comments
Comments must be written in English. Spam, offensive content, impersonation, and private information will not be permitted. If any comment is reported and identified as inappropriate content by OAE staff, the comment will be removed without notice. If you have any queries or need any help, please contact us at support@oaepublish.com.